Cervical Support Pillows Extend Your Treatment Value
October 11, 2023
Hiking Sticks for the Fall Season
November 10, 2023Is My Leg Pain Sciatica or Piriformis Syndrome?
Piriformis syndrome is a relatively common but often misunderstood neuromuscular disorder that can cause significant discomfort and pain. This condition primarily affects the piriformis muscle, a small muscle located deep in the buttocks, which plays a crucial role in hip rotation and movement. Piriformis Syndrome is often confused with true sciatica, and the origin can mistakenly focus on the lumbar discs.
What’s the Piriformis and how is it involved?
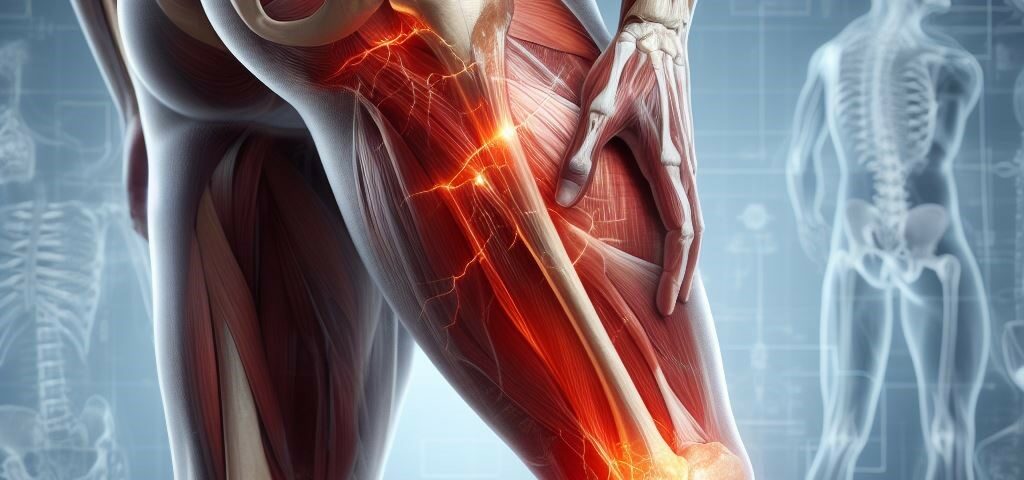
There is a set of small piriformis muscles on either side of the sacropelvis, running from the triangular sacral bone to the femur (upper leg bone). The Piriformis is a small player that helps to evert and abduct the leg, rotating the foot and knee outward and the leg up and back. The muscle sits close to the sciatic nerve, one of the largest nerves in the body, and in some cases, the muscle can irritate or compress the sciatic nerve. When this occurs, it can lead to the development of piriformis syndrome. Although it creates pain along the sciatic nerve, it is not a true “sciatica”. There is a really great animation of the piriformis and how it may impact the sciatic nerve here. The piriformis being in spasm will also potentially impact the Sacroiliac Joint (SI joint).
What are the Symptoms?
Symptoms of piriformis syndrome typically include pain in the buttock region that may radiate down the back of the leg, mimicking the symptoms of sciatica. This pain can be sharp, stabbing, or a dull ache and may worsen with prolonged sitting, walking, or certain activities that involve hip movement. The symptoms can be intense and impair your abilities, effect your sleep, and limit your work. There can be numbness in the leg and buttock – perhaps to the foot, low back pain, and maybe sacroiliac joint pain.
What is the Cause?
The exact cause of piriformis syndrome can be multifactorial. It may result from muscle imbalances, overuse injuries, trauma, or anatomical variations in the piriformis muscle or sciatic nerve. Diagnosis often involves a combination of clinical evaluation, physical examination, and occasionally imaging studies, such as MRI or CT scans, to rule out other potential causes of similar symptoms. It’s fundamentally important to have the right attention to the problem, before rushing to corticosteroid injections or surgery – this is where chiropractic can shine.
Why is it not “Sciatica”?
Sciatica is a term used to describe compression of the Sciatic Nerve most often from a lumbar disc failure, or a narrow lumbar canal. In Sciatica, the pain begins as a compression at the origin of one of the branch roots of the Sciatic Nerve, up in the lumbosacral spinal Area. In Piriformis Syndrome, the insult to the Sciatic nerve can be an irritation, friction or compression on one side in the lower buttock area. Compression on that buttock can often turn the pain on and off. Since Piriformis Syndrome often responds readily to non-invasive treatment, it is different from “Sciatica” which can often require a lot more attention, and certainly an MRI. While on the subject, we do also order MRIs and treat Sciatica at Blue Heron, in case you were wondering.
How can the pririformis be irritated?
A typical cause of Piriformis Syndrome is compression on the buttock, such as from the edge of a chair, sitting on a rock wall, or a fall. Occasionally, ladder work with the piriformis stretched tight can create irritation. Gait abnormalities, short leg syndrome, even bad footwear can cause or contribute.
Was Sciatica the Wrong Diagnosis?
It was close but not quite right. Quite often, we see patients who have been quickly diagnosed with Sciatica and even had a failed corticosteroid injection in the lumbar spine, because the problem is down lower, along the course of the nerve rather than the origin. They may have been chasing this problem for years. When these patients respond immediately to therapies, they are often shocked and surprised, but often quite pleased. At the same time, the sciatic nerve may also already be compressed from above, before it gets to the piriformis. We will rule that out up front.
What are Treatments for Piriformis Syndrome?
Treatment strategies for piriformis syndrome typically focus on improving function and structural dysfunction, erelieving pain and addressing the underlying causes. Remember, a chiropractor is like the referring MD and the physical therapist combined into one person; we do the exam AND the physiotherapies. These may include:
Chiropractic Manipulations are important: Gentle adjusting of the Lumbosacral Area, Pelvis, and Sacroiliac joint can help balance the tone of the piriformis by improving the structural function, and correct functional leg length issues which might also be causing the problem.
Adjunctive Physical Therapies: Therapeutic Ultrasound can help with irritation. Electrical muscle stim can bring down muscle spasm in the piriformis. The buttock is usually a bit too fluffy for Cold Laser to penetrate. Stretching and strengthening exercises can help improve muscle balance and reduce compression on the sciatic nerve.
Cold Hydrotherapy: Applying ice can help reduce pain and inflammation in the affected area. If we use heat in your treatment, we will finish with cold. We do not recommend heat packs for piriformis irritation.
Medications: Occasionally, anti-inflammatory supplements, Homeopathic muscle relaxants, other Non-steroidal anti-inflammatory drugs (NSAIDs) or muscle relaxants may be prescribed to alleviate pain and muscle spasms. Conservative therapies often try to avoid these.
Injections: Occasionally, providers will recommend or refer for Corticosteroid injections into the piriformis muscle or around the sciatic nerve may provide temporary relief. We rarely and actually almost never see this being necessary at our clinic.
Lifestyle Modifications: Adjustments in activities and ergonomics can help reduce aggravating factors.
Surgery: In severe cases when conservative treatments might fail, surgical release of the piriformis muscle or decompression of the sciatic nerve may be prescribed; this is rare unless in the case of an anatomical abnormality, like a sciatic nerve that developed to run directly through or in between the leaves of the pirifomis muscle. This occasionally occurs naturally as a body develops embryonically, and unfortunately can’t be diagnosed by an MRI. You probably don’t need to be concerned about this one, but we will keep it in mind.
Can I manage Piriformis Syndrome Myself?
Piriformis syndrome can be a challenging condition to manage – and definitely difficult to handle by yourself. It’s not a great idea to try and diagnose yourself, and treatment approaches can vary from person to person. Early diagnosis and a tailored treatment plan developed in consultation with a healthcare professional like Doctor Sibilla at Blue Heron Chiropractic can significantly improve the prognosis and quality of life for patients with this condition. Let’s talk about it before you head off for surgery or that Corticosteroid Injection!
Is Blue Heron Chiropractic masking for the COVID-19 Pandemic at this time?
Including with the latest COVID/Omicron variant, a lot of people are still getting sick. While it’s true that increased immunity has helped decrease the severity of responses in non-immune-compromised people, the sickness can still knock you out for a week or more. The Doctor is going to mask for your session. Your mask is definitely optional and we are absolutely fine with that. Staff is always vaccinated and boosted, and so even if we get this, we won’t be gone long and can get back to caring for you. We remain protective for folks who are immune compromised, have “Long Covid”, or need special considerations. A patient can wear their own mask at any time – and If you would like a mask and don’t have one, we can provide it – but again, masking is optional. If you have flu-like symptoms, are sneezing or coughing or blowing, we may provide you with a mask, so we can continue to serve you better; feel free to mention this to us when you call in to confirm your appointment. You can access Chiropractic safely and securely at Blue Heron Chiropractic & Healing Arts Center, with Dr. Dana Sibilla, DC DABCO FIANM.
Want some more chiropractic reading? Try our prior blog on Cervical Support Pillows.